Cardiovascular disease literally means disease of the heart and blood vessels, but it can cause additional life-altering complications that we might not initially associate with the disease, such as vascular dementia.
Vascular dementia is a decline in cognitive function resulting from damage to the network of blood vessels that supply oxygenated blood to our brains. In addition, reoccurring “mini strokes” – consequences of weakened vessel walls, leaks and bleeds, clotting, and narrowed arteries – temporarily block blood flow to parts of the brain. Tiny lesions caused by these brief interruptions may initially have little effect on brain function, but with time the damage accumulates and symptoms worsen.
Vascular Dementia vs. Alzheimer’s Disease
Vascular dementia and Alzheimer’s disease are the two most common forms of dementia. Alzheimer’s disease is characterized by a build-up of protein-rich amyloid-beta plaques and neurofibrillary tangles in the brain, as well as atrophy – or shrinkage – of brain tissue. Vascular dementia is not associated with disease specific protein accumulation or overall brain shrinkage. Instead, it is commonly characterized by areas of stroke-induced tissue necrosis or cell death. Alzheimer’s disease and vascular dementia are often found in the same individual.
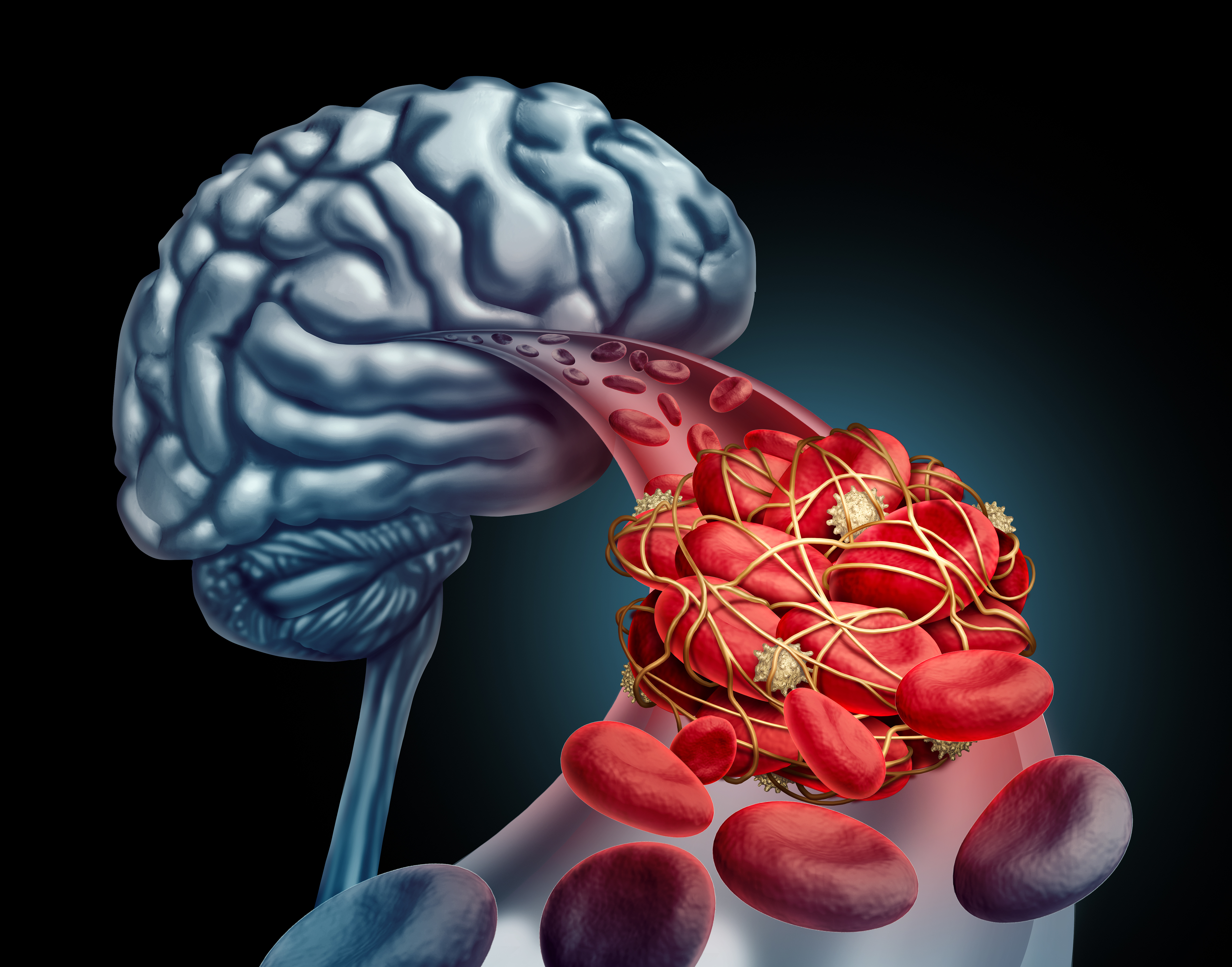
Symptoms of vascular dementia vary, depending on which areas of the brain are affected by the interruption of blood flow. “In contrast to Alzheimer’s disease, vascular dementia does not always present as memory loss.” says Dr. Jeffrey Cummings, Founding Director of the Cleveland Clinic Lou Ruvo Brain Health Center, Las Vegas and a world leading expert in the field of Alzheimer’s disease and dementia. “Some patients describe the early stages of vascular dementia as ‘something just not being quite right.’”
Sensory issues may arise first, such as poor depth perception. For others, issues with speech and language may be most noticeable. Some experience difficulty with planning, anticipating, and judging. For others still, general confusion, exhaustion, disorientation, frustration, or combinations of all of these cognitive manifestations may be what lead them to consult their doctor. This wide range of symptoms makes diagnosis of vascular dementia difficult, contributing to its under-recognition.
Limited Treatment Options
Currently there are no approved treatments for vascular dementia – and Alzheimer’s disease candidates that target plaques and tangles will be ineffective in vascular dementia.
“Drugs which target plaques and tangles in Alzheimer’s disease have so far failed in clinical trials. New treatment options with new targets have the potential to be successful in both Alzheimer’s disease and vascular dementia and need to be tested in clinical trials.” Dr. Cummings says about the current therapeutic landscape. “Targeting factors common to both vascular dementia and Alzheimer’s disease could yield a positive outcome in both areas.”
A New Approach to Treatment
One common cause of in Alzheimer’s disease, cardiovascular disease, and vascular dementia is vascular inflammation. Promising new evidence in Alzheimer’s research suggests that reducing systemic and local vascular inflammation may lead to positive outcomes. It’s also becoming well known that inhibiting vascular inflammation protects the heart and the brain, and lowering the risk of heart attack, stroke, and vascular dementia.
Inflammation is not the only process involved in injury or blockage of blood vessels. Vascular calcification works to harden arteries; plaques can form within vessel walls, impeding blood flow and delivery of oxygen and nutrients; and coagulation cascades are activated, leading to clot formation.
Dr. Cummings expressed his excitement about an approach targeting these underlying processes in cardio-vascular related dementia, “It’s very difficult, if not impossible, to treat only the brain in a non-invasive way. It makes logical sense that in diseases that are negatively affecting both the brain and body, we should be treating both. This is especially obvious in vascular dementia, where the cause of cognitive decline often originates from outside of the brain itself.”
Targeting Epigenetics
At the cellular level, disease-related factors are regulated by epigenetics – the mechanism by which genes are turned on and off to dictate how our cells function. As disease-causing genes are activated, harmful signals spread and more and more cells are pushed towards a diseased state. In cardiovascular disease and vascular dementia, this means that more processes are working together to damage the blood vessels and worsen patient outcomes.
“Developing therapeutics which operate on an epigenetic level is like going straight to the source,” says Dr. Cummings, “By a single therapeutic target at the epigenetic level multiple disease processes can be simultaneously improved. We’re dealing with multi-factorial problems, it’s time we start thinking about multi-factorial solutions”
The ongoing clinical trial, BETonMACE, includes monitoring of cognitive function in a pre-specified subpopulation of at risk patients. Results from these analyses will pave the way for a planned dementia-focused clinical trial.